PRACTITIONER
Medicine on the computer frontier
by Judith Stone
Judith Stone is senior editor at McCall's and co-host of the New York City cable-TV show Inside Travel.
About the only medical tasks not performed by computers are the cooking of chicken soup and the laying on of hands. It's not just the occasional maverick mavin adapting a personal computer to solve a specific problem, and it's not just the headline-making miracle cures. The plug-in practitioner is involved in almost every aspect of health care.
Chances are, you're already being diagnosed, drugged, dissected, debugged and dunned by computer. Doctors can call up your medical records on examining-room screens. They can monitor your blood with programs like the one at the University of Iowa Hospitals and Clinics that collects lab results, types labels, matches blood recipients and donors-and has cut potentially deadly human errors from eight a day to two a month.
Under the watchful electronic eye of a program like HELP, in use at the Latter-Day Saints Hospital in Salt Lake City, Utah, you would be safeguarded by an alarm that sounds when any treatment or drug appears to contradict information in its data banks. If images of your innards are required, you'll have a CAT scan (computerized axial tomography, a series of x-rays gathered and interpreted by computer).
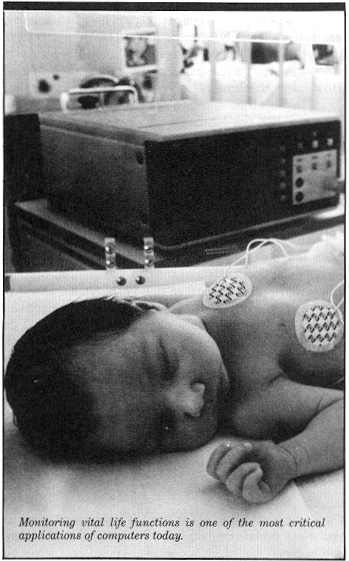
Should you need a new organ, a nationwide electronic network will find you a donor. Or maybe all that's needed is a boost from that internal computer, the pacemaker, which is nothing more than a microprocessor programmed to control heart rate. If surgery is required, you might spend twenty minutes at a terminal answering detailed questions that help your anesthesiologist choose the best possible medication. During and after the operation, your vital signs will be monitored by computer. And your bill will, needless to say, be processed electronically.
When you're handed a prescription, there's a good chance it's for a drug designed by computer. Until recently, researchers had to test thousands of compounds before they found one that did the job-say, hooking onto an enzyme created by a certain virus. Now computer graphics let scientists tinker with molecular configurations on the screen, not in the test tube; finding the right one takes weeks, not months.
Your pharmacist may keep computerized files like those developed by the Giant Food chain of Maryland for its thirty-two pharmacies. The druggist can instantly see what other medications you're taking and check for potentially dangerous interactions, print labels with special instructions based on your medical history, make sure when he issues a refill that you haven't been using up the drug too fast, fill out insurance forms, bill you and give you a printout for your tax records.
Micro Miracles
An estimated ten thousand computers are at work in medicine, 60 percent of them personal micros. Machines monitor every bodily process from fluid intake and outgo to the speed of a man's sperm (important for infertile couples). Silicon specialists swiftly interpret tests, from electrocardiograms to psychological inventories. Environmental control programs are revolutionizing rehabilitation. The disabled can switch on fans, turn the pages of books, dial the telephone-in some cases using computers equipped with a speech-recognition device that responds to spoken commands.
Ron Steele suffers from a degenerative neurological nightmare that has locked a fine, probing mind in an increasingly helpless body. Last year amyotrophic lateral sclerosis (ALS), "Lou Gehrig's disease," robbed him of the ability to speak and write. Ron could communicate only by laboriously spelling out words, pointing to an alphabet card with a wand held in his mouth. Today he's chatting nonstop, sprung from solitary by a specially programmed Texas Instruments personal computer that lets him fill the screen with messages as fast as he can send Morse code, using a switch taped to his eyebrow. He can write, issue a variety of commands and activate the printer.
The program was devised by Gregg Doty, president of CompuTech Distributing in Springfield, Missouri, and senior staff programmer Edward Cooley. Doty and Cooley recall that Ron was initially suspicious of the small machine and reluctant to try it. A day later, nurses couldn't get him to leave it alone. Ron's first message after mastering the code was a loving letter to his wife, coordinator of nursing education at Missouri State Chest Hospital, where he is a patient. An unexpected bonus has been that his six children, for whom visits were once painful and confusing, now spend hours crowded around the computer with a dad radiating obvious joy at being able to play with them again.
Computers play a part in prevention, too. For example, with a program called Plato Staywell, designed to help people manage hypertension, lose weight and quit smoking, users can practice ordering low-cal, low-sodium meals from a simulated menu, then rate their picks. But perhaps the most important medical applications of computers will come in information management, billing and record keeping, and high-tech healing straight from Tomorrowland.
Experts estimate that internists who want to practice good medicine must know about a million facts-two million if they're specialists. The only way doctors can keep this ever multiplying data at their fingertips is by keeping their fingertips applied to a computer keyboard, tapping into the one hundred or so medical data bases available or using "expert" programs that access and diagnose illness just the way a human practitioner does.
Supersmart systems work in several ways. Rulebased inference uses an "if this, then that" pattern. With statistical pattern recognition, the program tells you the probability that a proposed diagnosis is the right one. Data bases compare one patient against others with the same problem. Such a program is used at Pinderfields Neurological Centre in Wakefield, England, to determine which patients with head injuries should be scanned for hematoma (blood clot). Given information about the patient's condition, the computer checks it against a data base to determine the percentage of risk. Doctors estimate that they can eliminate three hundred deaths a year with the computer.
Cognitive models come the closest to reproducing human thought processes. Given a set of symptoms and lab reports, the computer makes what doctors call a differential diagnosis, asking pointed questions to narrow the possibilities until a diagnosis is reached. CADUCEUS, developed at the University of Pittsburgh and originally called INTERNIST-1, is such a program; it's the star of SUMEX-AIM (Stanford University Medical Experimental Computer for Artificial Intelligence in Medicine), a mainframe funded by the National Institutes of Health. Fed your symptoms and lab results, CADUCEUS quickly skims its data bank of 4,000 manifestations of 600 diseases, asking question after question to pinpoint a diagnosis. The program CADUCEUS did just as well as human general practitioners in a test of diagnostic skills-but not as well as specialists.
Other supersmart systems include two Stanford programs: MYCIN, which helps decide which antibiotic will best treat infections, and Project Rx, which may someday make medical discoveries of its own. Rx examines patient records for cause-effect relationships, makes hypotheses in the form A causes B, then tests the hypothesis against patient records and statistics. In one test the computer checked out seventeen hundred patients and was able to develop its own causal theories of disease. Most of what it found has already been described in the medical literature, but new discoveries are possible. ATTENDING is a program that critiques residents in anesthesiology; ONCOCIN suggests the best treatment for cancer patients. AI/ RHEUM, developed by Rutgers and the University of Missouri, helps nonspecialists in the diagnosis of twentysix rheumatic diseases.

Computers also help doctors cope with information overload by allowing them to hone their skills through game playing. Using AMA/NET, the telecommunications network of the American Medical Association, they can quiz a simulated patient (played by a computer at Massachusetts General Hospital), suggest a diagnosis and have their problem-solving techniques critiqued by the computer. There are twenty modules in different medical specialties and of increasing difficulty; doctors can send questions or comments to the MGH computer via an electronic mail system. Originally developed for the Harvard Medical School, the programs give isolated physicians a chance to continue their education.
Physicians in private practice use computers mainly for billing, record keeping and word processing. While it may not thrill you to know that billing by computer is five to twenty times faster than manual billing and much more accurate, it's nice to know that if, say, a drug is recalled, doctors can swiftly scan their patients' charts, locate those using the drug and contact them immediately. Also, computerized records can be easily transferred to a specialist or hospital. And some legal experts have pointed out that detailed computerized medical records can help doctors defend themselves in malpractice suits, thus eventually bringing down medical costs.
Most medical programs for billing, record keeping and information management are written in a computer language called MUMPS (Massachusetts General Hospital Utility Multi-Programming System), created in 1969 by Dr. G. Octo Barnett of the hospital's Laboratory of Computer Sciences. MUMPS handles medical information five to ten times faster than any other computer language; it can randomly access a large data file, lends itself to arrays and tables, processes words and is easy to learn.
Digital Doctoring
Among the flashiest pieces of Star Wars hardware are the big scanners that provide more detailed pictures of the inside of a human body than anyone thought possible. The first of these was the CAT scan, designed in 1973 for imaging the brain. X-rays from various angles give a cross-sectional picture of the body. The PET scan (positron emission tomography) makes computer images from radioactive isotopes placed inside the patient and actually catches the body in the act of metabolizing. The Cine-CT scanner, developed at the University of California, San Francisco, shoots twentyfour electron-beam images per second to measure the movement of the heart, cardiac wall thickness and rate of blood flow. And a technique called nuclear magnetic resonance is especially exciting because it doesn't use radiation. Magnetic fields passed over the body cause cell nuclei to emit faint radio waves that are then monitored by computer; it looks as if NMR may reveal the presence of cancer.
Computers are replacing and revitalizing worn body parts. A device developed at Johns Hopkins, the Implantable Programmable Infusion Pump (IPIP), is a computerized insulin pump placed just under the skin of the abdomen. The unit, three and a half inches in diameter, contains an insulin reservoir that can be filled every few months by injection. Radio waves link the pump to a physician's computer terminal. The doctor can reprogram the amount and rate of insulin being pumped by holding a computer-controlled transmitter over the patient's belly and communicating with IPIP the way Mission Control commands satellites.
Nan Davis, now twenty-four, was left paralyzed from the waist down after a car accident on prom night, yet she walked up to receive her diploma from Wright State University in Dayton, Ohio. Her legs do their work with a boost from a computer-powered machine designed by Jerrold S. Petrofsky of the school's Biomedical Engineering Laboratory. The apparatus sends electrical signals to the fifty or so muscles that work at walking, bypassing the damaged part of Davis' spinal column. Sensors on her legs, feet and shoes let the computer know how she's doing. And Davis isn't the only paralyzed person stepping out-and even bicycling-under computer power. A few hundred miles from where Nan Davis walked, at Case Western University in Cleveland, researchers have made paralyzed arms move by implanting electrodes directly into hand muscles. Electrical signals sent from a computerized transmitter make the muscles move smoothly enough to let patients eat, brush their hair and use the phone.
Computer graphics are helping to redesign the human body. A new program allows plastic surgeons to manipulate simulated bones and flesh to get a clearer idea of what a proposed facial reconstruction will look like-and how they can do the job most efficiently. CAT scans give cross-sections of the skull, but what plastic surgeons need is a 3-D picture. So researchers at St. Louis Children's Hospital developed a system that essentially stacks cross-sections to yield a 3-D picture. CASPR (Computer-Aided Surgery Project) lets surgeons play with a 3-D skull to see how patients would look if different parts of their face were moved around.
Pros and Cons
So what does it all mean? There are those who think computers will dehumanize medicine. The medicos ex machina, they say, will be even harder to relate to than the already icily Elite class that commands us to say ah. These critics maintain that the cosmic mystery at the center of medicine, the power of healing, defies quantification. The human body is highly idiosyncratic; its workings can never be reduced to binary code. Diagnosis is at bottom intuitive, requiring a keen eye and an inspired touch. A machine just doesn't have the requisite psychic energy; doctor as shaman, computer as sham.
Will patients get enough of a doctor's attention in the digital age? In the electronic office, where the only paper is last year's magazines in the waiting room, who will care for us? Then there's the problem of privacy: the antics of the 414 gang, the hackers who trespassed on Memorial Sloane Kettering's patient files, proved that hospital records can be tampered with-a threat to patients more sinister than human error.
On the other hand, there are those who think computers will rehumanize medicine. No longer asked to be walking libraries, doctors can spend more time with patients. Computers can handle the mindless statistical searches, leaving doctors free to explore what's unique about individual cases. Without digital assistants, doctors won't be able to keep up and serve well. Moreover, studies have shown that some people feel more comfortable and more in control when they confide in computers instead of people.
Computers save us money, build us spare parts, reduce potentially fatal human errors and detect disease with astonishing efficiency. How bad is that?
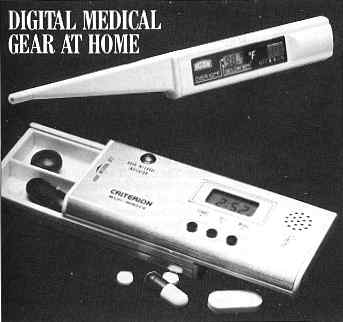 Dedicated microprocessors have opened the way for "smart" medical gadgets to be used in any home: not expensive lifesaving equipment like pacemakers or portable dialysis machines, but relatively low-cost "intelligent" versions of traditional medicine cabinet staples. The electronic digital fever thermometer is the most precise thermometer available for home use, providing a digital readout accurate to within one-tenth of a degree (Fahrenheit). Measures temperatures within sixty seconds (instead of the customary three minutes for glass thermometers); chirps when temperature is reached and sounds alarm when high fever levels are indicated. Registers oral, rectal or underarm temperature. The digital alarm pillbox (weighing in at two ounces) has an automatic repeating timer alarm that can signal at intervals of one-half, one, two, four, eight or twelve hours as a reminder for taking medication. The built-in microprocessor-driven digital clock has a separate wake-up alarm and month/day calendar. |
Return to Table of Contents | Previous Article | Next Article

